ANN ARBOR – Michigan’s rural hospitals are entering a more dangerous phase of financial stress—driven by rising healthcare costs, growing numbers of uninsured patients, and mounting federal budget pressure tied to global conflict.
What was, just weeks ago, a policy concern is increasingly becoming a real-world risk.
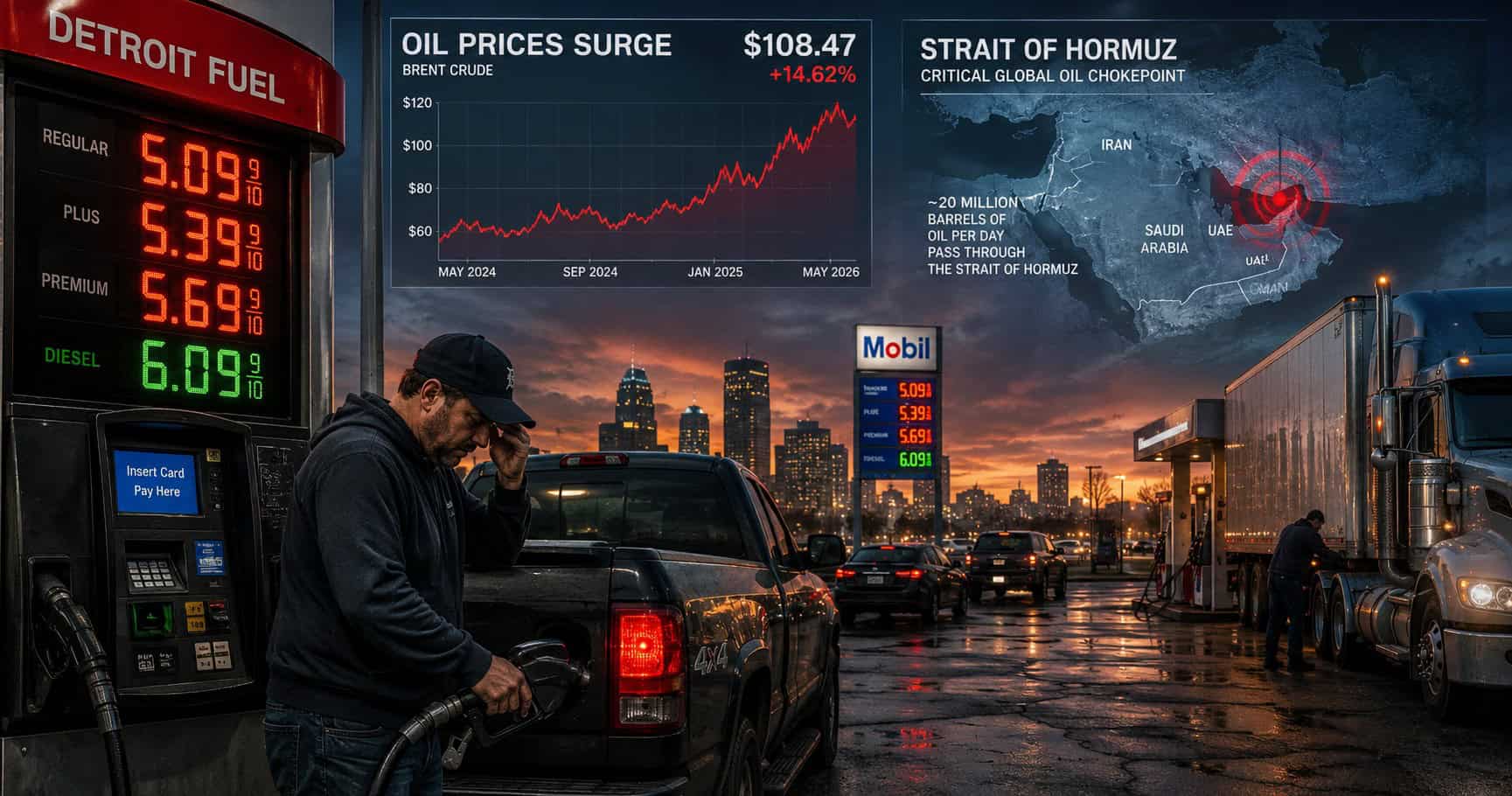
With the Iran war now stretching into its second month and costing an estimated $1 billion to $2 billion per day—and the Pentagon seeking hundreds of billions in additional defense funding—pressure is building on federal finances. That pressure is expected to ripple into domestic spending, including healthcare.
Hospital leaders across Michigan say the strain is already visible.
At Scheurer Health in Michigan’s Thumb region, CEO Dr. Ross Ramsey warned rural hospitals are “reaching a brink of collapse,” pointing to rising costs and heavy reliance on government reimbursement programs.
“We tend to have higher Medicare and Medicaid rates… over two-thirds of our revenue stems from government programs,” Ramsey said. “When they’re cutting back… you really take a hit.”
The Cost Equation Is Getting Harder to Ignore
The scale of current military spending is beginning to reshape the broader fiscal landscape.
At up to $2 billion per day, the cost of the Iran conflict is rapidly approaching the scale of major domestic programs. At the same time, federal policymakers are weighing significant increases in defense spending—reportedly in the range of hundreds of billions of dollars.
That combination is forcing difficult tradeoffs.
Healthcare is politically sensitive and unlikely to face sweeping cuts. But historically, sustained military spending at this level leads to tighter constraints on domestic programs, including slower funding growth, reimbursement pressure, and reduced flexibility in programs like Medicaid.
For rural hospitals, those incremental changes can carry significant financial consequences.
Rural Michigan Hospitals Already Operating on Thin Margins
Even before current geopolitical and budget pressures, many rural healthcare providers in Michigan were struggling to stay afloat.
Key challenges include:
- Low patient volumes limiting revenue
- Higher rates of uninsured or underinsured patients
- Workforce shortages, particularly in specialized care
- Heavy reliance on Medicaid and Medicare reimbursements
Data from rural health organizations suggests that roughly one-third of Michigan’s rural hospitals are already operating with negative margins.
Unlike large urban systems, rural hospitals often lack the scale and financial reserves needed to absorb rising costs or fluctuations in reimbursement rates.
Some have already reduced services. Others are quietly evaluating long-term sustainability.
Now, those pressures are intensifying.
Closures Haven’t Hit—But the Warning Signs Are Flashing
Michigan has not yet experienced a new wave of rural hospital closures in 2025 or early 2026. However, multiple analyses indicate that a meaningful number of facilities are financially vulnerable.
Estimates suggest that between 10 and 13 rural hospitals in the state are at risk of closure, with several considered in immediate financial danger based on current operating conditions.
Among those frequently cited in policy discussions and reporting are:
- McLaren Central Michigan
- UM Health–Sparrow Carson City
- Ascension Borgess-Lee
But Linda Reetz, U-M Health Regional Market President, who oversees community hospitals such as U-M Health-Sparrow Carson, disagreed with the reporting.
“UM Health-Sparrow Carson (formerly Carson City Hospital) has been serving this community for 90 years and will continue to be the safety net for health care, providing access close to home,” she said.
“We are proud to say that UM Health-Sparrow Carson is thriving, and our inpatient volumes are at the highest point they’ve been at for well over a year. We have added specialty services for our patients, including orthopedics, general surgery, urology, and Women’s Health to name a few. We have also reinvested in building infrastructure and renovations to ensure a healthy, safe and welcoming environment.
She added: “Our work is not done as we have plans to add additional specialty services for our patients and are more committed than ever to keeping care close to home.”
Hospital Leaders Warn of System Strain
Executives say the issue is not limited to individual facilities—it affects entire regional systems.
In the Upper Peninsula, Tonya Darner, CEO of UP Health System, said even small funding changes can create cascading problems.
“Reducing the funding doesn’t erase the need,” Darner said. “I need all of those hospitals across the U.P. to stay open… I don’t have the capacity to care for all of the patients.”
Healthcare leaders say the stakes extend beyond finances.
“Rural hospitals are usually the hub of the community,” said Wendy Frush, CEO of Munising Memorial Hospital, underscoring the role these facilities play in local economies and quality of life.
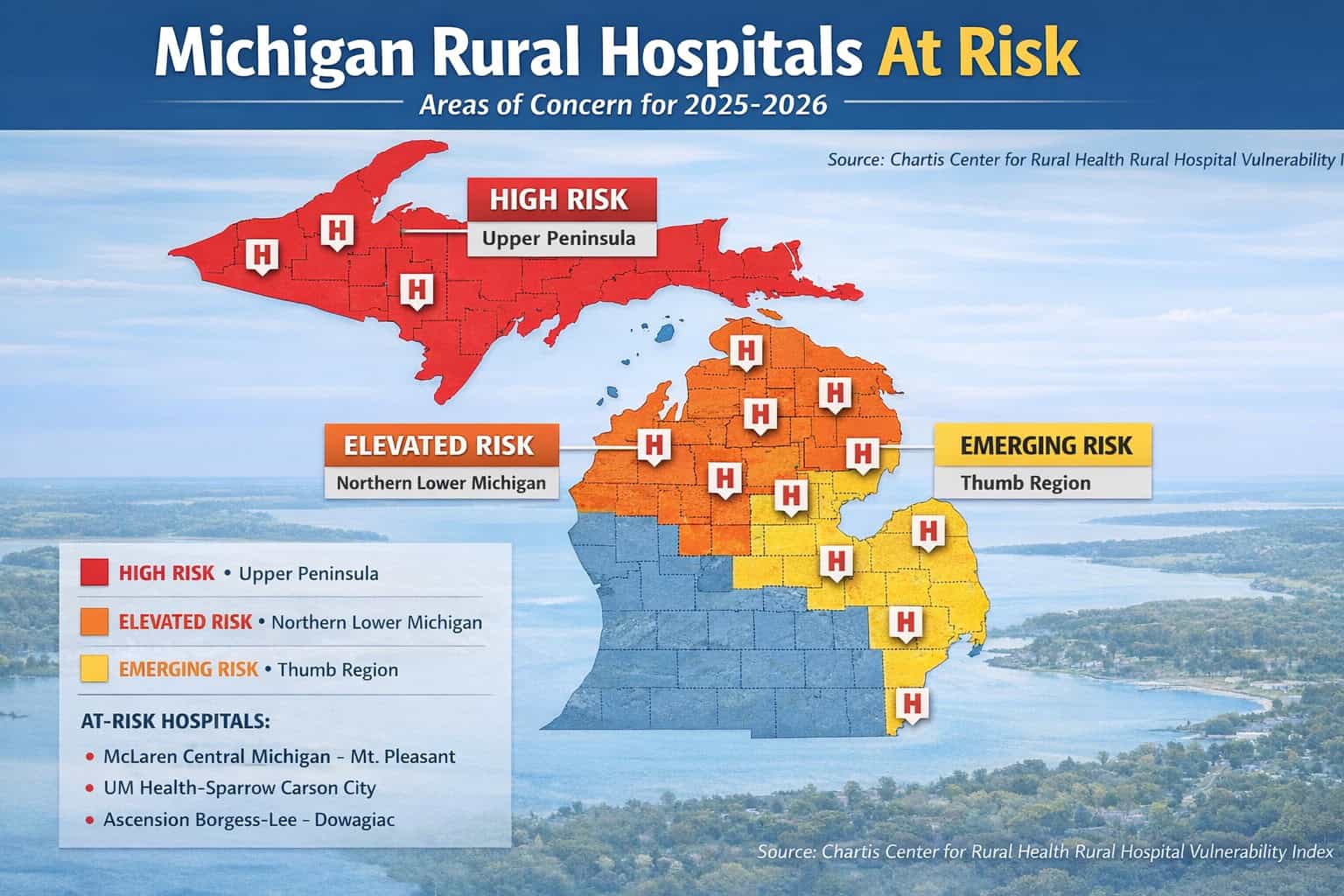
Where the Risk Is Highest in Michigan
The financial pressure facing rural hospitals is not evenly distributed across Michigan.
Healthcare analysts point to three regions where the risk is most concentrated: the Upper Peninsula, the northern Lower Peninsula, and parts of the Thumb.
In the Upper Peninsula, low population density and geographic isolation create structural challenges that make hospital operations particularly difficult. In northern Michigan, hospitals face quieter but persistent financial strain tied to workforce shortages and seasonal economies. In the Thumb, higher rates of uninsured patients and reliance on Medicaid increase exposure to reimbursement pressures.
Several hospitals—including McLaren Central Michigan, UM Health–Sparrow Carson City, and Ascension Borgess-Lee—have already been identified as financially vulnerable.
While full closures have not yet accelerated, some hospitals are scaling back services or eliminating inpatient care, reducing access even when facilities remain open.
Uncompensated Care Is Adding New Financial Stress
Another pressure point is growing inside rural hospitals: uncompensated care.
As insurance costs rise and coverage becomes less stable, more patients are delaying routine treatment and turning to emergency rooms when conditions worsen. Under the Emergency Medical Treatment and Labor Act, hospitals are required to provide emergency care regardless of a patient’s ability to pay.
However, reimbursement is often limited or nonexistent.
Emergency care is among the most expensive services hospitals provide. When those costs are not recovered, losses accumulate quickly—particularly for smaller facilities with limited financial reserves.
Hospital administrators say even modest increases in uninsured patients can significantly impact financial stability.
Rising Costs Are Hitting From All Sides
At the same time federal budget pressures are building, healthcare systems are dealing with immediate financial strain.
Insurance premiums are rising in 2026, driven by inflation, higher utilization, and the expiration of enhanced federal subsidies. Employers are absorbing some of those increases—but are also passing more costs on to workers.
That has a direct impact on rural hospitals.
As out-of-pocket costs rise:
- Patients delay or skip care
- Emergency visits increase
- Uncompensated care grows
This creates a feedback loop that weakens hospital finances even further.
Why Rural Hospitals Are More Exposed
Rural hospitals sit at the intersection of multiple vulnerabilities.
They depend more heavily on:
- Medicaid reimbursements
- Federal and state support programs
- Stable insurance coverage within their communities
When any of those factors shift—even slightly—the financial impact is magnified.
If federal budget pressures lead to tighter Medicaid funding or slower reimbursement growth, the effect on rural providers can be immediate.
A Ripple Effect Across Local Economies
The financial health of rural hospitals is closely tied to the economic health of the communities they serve.
Hospitals are often among the largest employers in rural areas. When they reduce services or scale back operations:
- Jobs are lost
- Local businesses see reduced economic activity
- Community stability is affected
Access to healthcare also plays a key role in attracting and retaining workers, making hospital stability a broader economic issue.
A Growing Issue for Voters
Healthcare access has long been a defining issue in rural communities, where hospitals often serve as both essential care providers and major employers.
As financial pressures build, reductions in services—or potential closures—can have an immediate impact on daily life.
Issues tied to cost of living and access to essential services, including healthcare, tend to resonate strongly with voters in these regions.
A Slow-Building Crisis With Real Consequences
There is no single breaking point—at least not yet.
Instead, the risk lies in a steady accumulation of pressures:
- Rising healthcare costs
- Growing uncompensated care
- Federal budget constraints
For rural hospitals, that gradual squeeze can be more dangerous than a sudden shock.
As war costs mount and federal priorities shift, the financial pressure is beginning to move through the system.
In Michigan, rural hospitals are among the first places where those pressures are likely to be felt.
And for the communities that depend on them, the stakes are rising.